It’s no exaggeration to say that effective data collection is a cornerstone of a robust regulatory strategy under the MDR.
So much of working with the EU MDR concerns the harvesting, identification, appraisal and analysis of clinical evidence that, in the absence of effective data collection systems, the whole framework can become inefficient with ongoing regulatory approval becoming highly problematic.
Post-Market Clinical Follow-Up (PMCF) and Vigilance systems are vital components of Post-Market Surveillance (PMS) systems under the EU MDR. In this article, we consider steps that manufacturers can take to drive compliance with PMCF and vigilance data collection.
The following ‘golden rules’ guide all of our PMCF design services and underpin our success in driving ongoing investigator engagement and data collection compliance. For further information about our approach to maximising data collection compliance, speak with a member of our team.
Effective data collection - the golden rules
Whatever the type of clinical data being collected - whether it’s PMCF data, complaints, or inputs into a formal clinical trial - there are several ‘golden rules’ that help maximise data collection compliance. In turn, adherence to these rules can help ensure that you have access to the clinical evidence you need for ongoing approval of your device.
1. Keep it simple
Perhaps the most important of all of the golden rules, it’s vital to keep datapoints simple and streamlined. It’s so tempting to add more and more datapoints, reasoning that the study will have more ‘value’ if questions are granular and detailed. In reality, time-consuming data entry forms are the quickest way to reduce data entry compliance and the worst way to encourage investigators to continue engaging with the study.
Rule 1 - Data points should be reduced to the minimum required to fulfil the objectives of the study. Questions should be simple to understand, unambiguous, and quick to answer. Unnecessary detail should be entirely eliminated.
2. Make data entry easy and convenient
Too many manufacturers rely on cumbersome, paper-based data collection systems. Paper based data entry suffers from numerous flaws that, in turn, will lead to patchy data collection. These flaws include:
- Paper can get lost or damaged and can easily fall into the wrong hands.
- Paper is slow to work with and must eventually be transcribed into a digital format for analysis, introducing a source of error or bias.
- Paper must either be physically transported from the clinical site to the study sponsor (or nominee) or digitally transcribed on-site, introducing a further reason for poor investigator compliance.
Well-designed digital data collection platforms overcome all of these problems and introduce a level of data security that is impossible to achieve with manual systems.
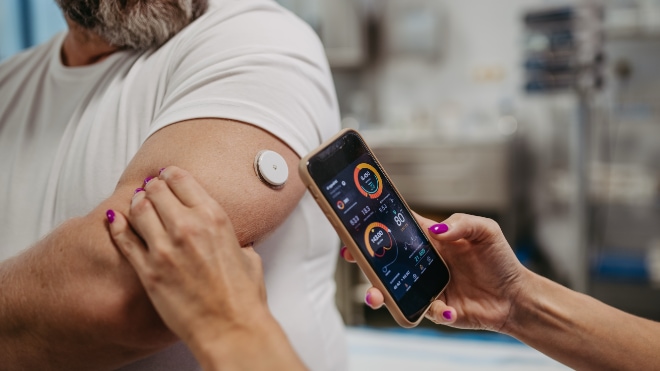
Rule 2 - Data collection should be through dedicated digital systems that are designed specifically for handling clinical data. They should be incredibly simple to use and should function from smartphone, tablet or computer. They should have low data and processor requirements and should not lag or fail. Digital data storage should adhere to the highest recognised standards relating to the handling and storage of clinical data.
3. Reward and support investigators
Clinical investigators are busy people. The truth is that every time a clinician or user enters data relating to your device, your are indebted to them for their efforts. Too many manufacturers begin to take investigators for granted; especially (and somewhat counter-intuitively) those who are the most prolific data enterers. This stems from the idea that compliant investigators will ‘take care of themselves’ and that efforts should focus on those who are proving troublesome to get up and running with the study. This is the wrong approach. In reality, 80% of your data will likely come from 20% of your investigators, and it is these who should be thanked, rewarded (compliantly) and encouraged.
Rule 3 - Focus on your best investigators and ensure they know that their efforts are appreciated. Do everything you can (compliantly) to demonstrate your ongoing gratitude for their efforts.
4. Ensure that follow-up requirements are reasonable
When designing clinical studies, it is tempting to plan for long-term follow-up of subjects that far exceeds that normally encountered in clinical practice. The allure of this is easy to understand - outcomes at ten years post intervention can generally be held to be more definitive than those at six months.
However, long-term follow-up requirements are a sure-fire way to find compliance with data entry waning over time. Before you know it, your ten-year follow-up study could have only a small percentage of investigators and subjects still participating in the study only a proportion of the way through its planned duration. While a reasonable middle ground will usually need to be found, it’s much better to have high compliance to a shorter follow-up than poor compliance to a longer one.
Rule 4 - Ensure that follow-up periods are sensible, appropriate and easy for investigators and subjects to work with.
Summary
These are some of the guiding principles behind the way we construct PMCF systems for our clients from across the industry. To find out more about our approach to PMCF and data collection in general, contact a member of our team for a no-obligation discussion.
This is Part 3 of our PMCF under the MDR article series. Subscribe to our Newsletter to ensure you don’t miss any of this comprehensive series.